YOUR BUSINESS AUTHORITY
Springfield, MO
YOUR BUSINESS AUTHORITY
Springfield, MO
Missouri is one of 14 states that has not adopted Medicaid expansion since the coverage became available six years ago.
Debate has stalled for years over the issue, mainly stemming from funding concerns by the state’s Republican-majority legislature. But after an initiative petition was filed in May, the decision to expand health care coverage is headed to Missouri voters.
Initially set for the November election, Gov. Mike Parson signed a proclamation on May 26 that expedited the ballot measure for the Aug. 4 primary.
“I want to be clear that this is about policy, not politics,” Parson said in a news release. “At a time when our state is undergoing a major health, economic and budget crisis, we need to know exactly where we stand on what would be a massive spending initiative for Missouri.”
Parson, a Republican, called Medicaid expansion a “massive tax increase that Missourians cannot afford” in his State of the State address in January, adding it would come at the cost of education, workforce development and infrastructure costs.
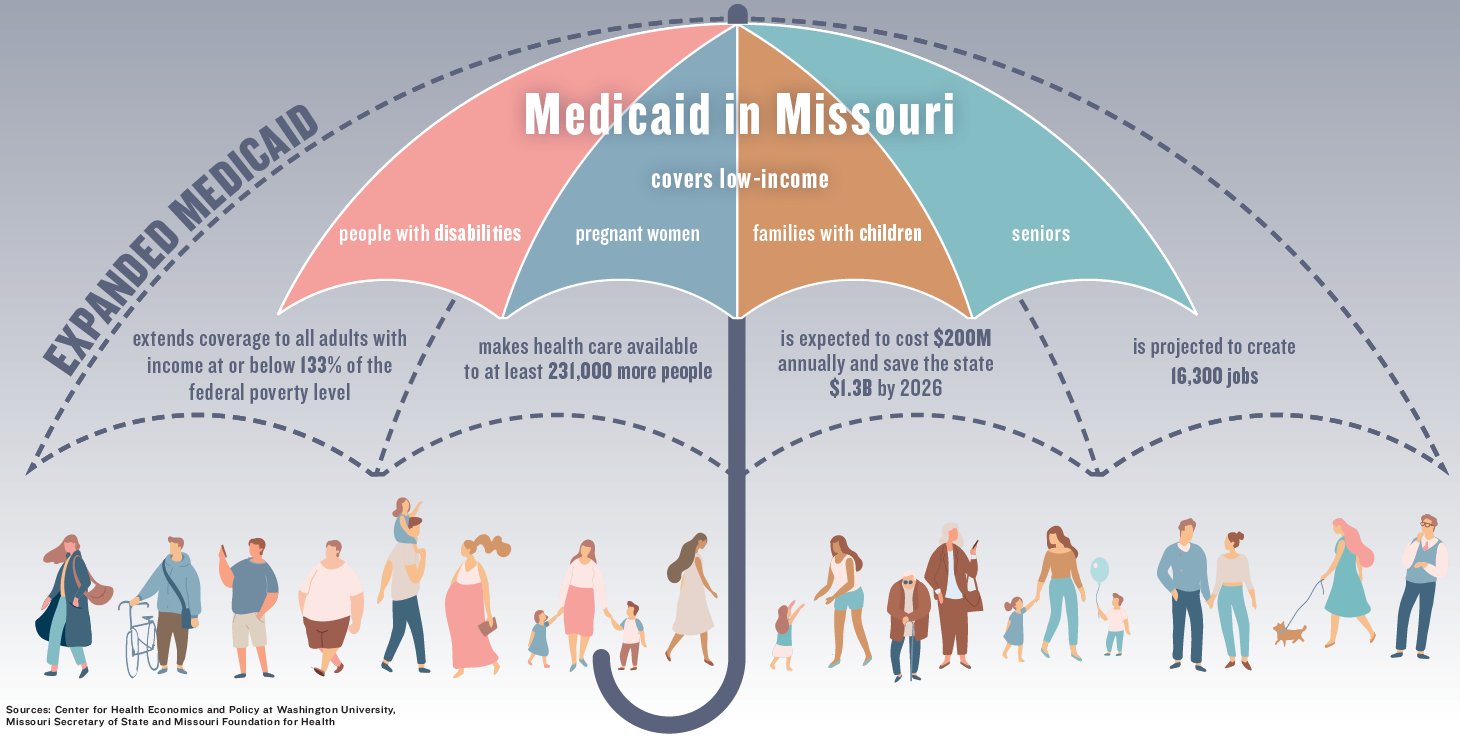
If passed, coverage would be extended to individuals between the ages of 19 and 65 that have annual income at or below 133% of the federal poverty level, according to the ballot language. That’s roughly $17,000 per year for an individual or $29,000 for a family of three. Currently, the state’s Medicaid program, MO HealthNet, is only available to low-income individuals in four categories: those with disabilities, families with children, seniors and pregnant women. There were over 923,000 enrollees in May, according to the Missouri Department of Social Services.
A study published by the Center for Health Economics and Policy at Washington University in St. Louis found that Medicaid expansion would help roughly 231,000 additional people in Missouri get access to health care. Contrary to the governor’s assessment, the study finds the program would be revenue neutral and could create cost savings for the state of up to $1.3 billion by 2026. The study cited additional federal dollars offsetting the current state expenses. Missouri’s share of Medicaid costs is 35%, but if expanded, that would drop to 10% with the federal government contributing 90% of the costs.
The expanded program became available in 2014 under the Affordable Care Act, which was passed into law in 2010 by President Barack Obama. States were initially expected to adopt Medicaid, but a U.S. Supreme Court ruling in 2012 made it optional.
Medicaid expansion in Missouri is backed by such organizations as the state chamber of commerce and the Missouri Hospital Association. Matt Morrow, president of the Springfield Area Chamber of Commerce, declined to comment on the ballot issue.
Local health care leaders have come out in support of expanding the program, who say it would direct more dollars to the health care systems and make preventative care more accessible to childless adults between the ages of 19 and 65. Both CoxHealth and Mercy leadership say they lose tens of millions of dollars each year on Medicaid and charity care that is not reimbursed.
Rep. Crystal Quade, D-Springfield, predicts voters will approve the measure in August, based on support she’s heard from local constituents.
“I have no doubt it will pass overwhelmingly,” Quade said. “It’s something we should have done when we first had the opportunity. … Initiative petitions are the last stop that voters have outside of elections to hold us accountable.
“(Medicaid expansion) coming by a vote of initiative petition, showed me that we have failed.”
According to an SBJ.net poll taken June 19-25, 61% of the 425 respondents said they would vote for Medicaid expansion in August.
Crunching the numbers
Funding has long been at the epicenter of the Medicaid debate in Missouri, said Sen. Lincoln Hough, R-Springfield, who serves as vice chair on the senate’s appropriations committee.
According to the ballot language, extending the health care coverage is expected to increase costs of at least $200 million annually through the state’s contribution to the federal program compared to $1 billion in savings by 2026.
Hough said the potential costs can’t be overlooked by a legislature that passes a constitutionally mandated, balanced budget each year.
“Two hundred million [dollars] out of a $30 billion budget doesn’t sound like much money, but it’s roughly 2% of annual general revenue growth,” Hough said. “The number we were budgeting last year, prior to COVID-19, was around 1.7% of growth … so expanding Medicaid could potentially eat all of the economic growth for a year.”
Hough said it’s also likely that more than 231,000 people sign up for the program, which would lead to further budget cuts. According to U.S. Census data, 11.2% of Missouri citizens under the age of 65 are uninsured, which is roughly 571,000 people.
Though studies have found that expanding Medicaid also would lead to job creation in the ballpark of 16,300 positions, Hough is concerned the legislature would continue to reduce income taxes.
“We have a certain segment of parties that believe you can cut your way to prosperity, and we have an income tax that’s barely over 5%,” he said. “At some point, we do have to have some tax revenue to pay for the services people expect to have in the state.”
Parson said in a news release that placing the initiative on the August ballot would allow the state more time to prepare for the budget impact.
Quade said lawmakers have attempted to pass measures that would increase general revenue, like the so-called Wayfair use tax of online sales from out-of-state retailers, though the efforts have failed.
“The state of Missouri is in a financial crisis right now,” she said. “(COVID-19) has impacted that, but also have the policies that we’ve seen over the past 10 years where we’ve been giving corporate tax breaks left and right.
“The two places we go when we are needing money are education and health care. We’re continuing to see vulnerable populations on the chopping block.”
Preventative care
Both CoxHealth and Mercy leadership say the hospitals would see more patients with expanded Medicaid.
“People who don't have the insurance, they wait until they're more acutely ill, and then they go to the ER – but what they miss out on is the ounce of prevention,” said CoxHealth CEO Steve Edwards. “If we can get patients to get into primary care, the hospital, the patient and the state saves money.”
Medicaid currently pays about 65% of the cost on straight claims to hospitals, he said, and CoxHealth writes off hospital bills for uninsured patients as charity care. Edwards posted on Twitter in February that charity and uncompensated care hit $232.8 million in 2019, up 19% from the year prior.
On average, CoxHealth reports losing roughly $36 million a year in nonreimbursed Medicaid costs. Edwards said the system would still lose some money with the expanded program, but it be would a smaller dip in the hospital’s bottom line, which is generally 1%-3%. CoxHealth recorded $5.1 billion in 2019 revenue and placed No. 9 in SBJ’s 2020 Dynamic Dozen.
Craig McCoy, president of Mercy Springfield Communities, said the health care system recorded $53 million in charity care and $25 million in Medicaid shortfalls in fiscal 2019.
He said the $53 million in charity care would largely go away with Medicaid expansion, as more patients would be insured.
“By not being a Medicaid expansion state, those dollars are going to the other states that have expanded,” McCoy said, adding the increase of MO HealthNet patients would lead to job growth at the local hospital system which recently reported nearly 700 cuts and furloughs amid the COVID-19 pandemic.
McCoy and Edwards both hope voters pass the measure, adding recent events identify a need for health care.
“In a pandemic, we better realize what it means as a community and as an entire state for people not to have care,” Edwards said.
Moseley’s Discount Office Products was purchased; Side Chick opened in Branson; and the Springfield franchise store of NoBaked Cookie Dough changed ownership.